Black Spot Under Toenail
5) benstevens / Thinkstock
Why Are My Toenails That Color?

Whether you’re washing your hands or admiring a manicure, you spend a lot more time looking at your fingernails than your toenails. Maybe it’s time to focus on your feet more often (and not just during sandal season). Toenail color changes — from a big blue spot to a thin brown line — could signal health problems. Here’s what you need to know.

Black Toenail: Common Causes
2/11
If your toenail turns black, it’s most likely a bruise under the nail, technically called a subungual hematoma. You can get it from stubbing a toe or from footwear that cram your feet into the front of the shoe. The bruise usually starts out red, then becomes purple, dark brown, and finally black when blood beneath the nail pools and clots. Expect your black toenail to grow out in about 6 to 9 months or longer.
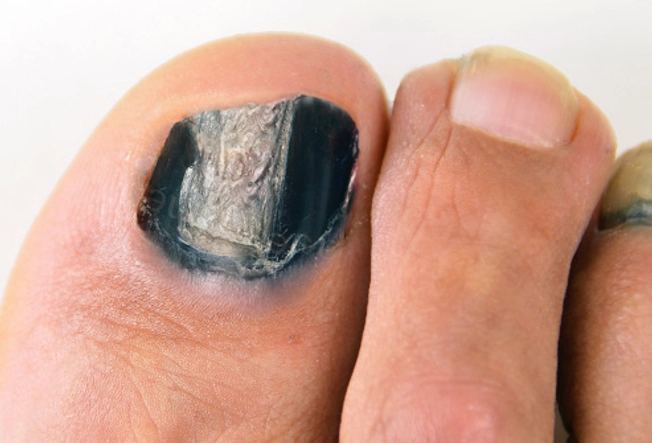
Black toenail: Rare causes
3/11
Say you’re not a runner, your shoes are roomy, and you’re sure you haven’t hurt your toe — yet you have one or more black toenails. Check to see if it’s just that dye has rubbed off from a pair of shoes. If not, head to the doctor. You might have a rare cause of black toenail, such as:
- Malignant melanoma, a serious form of skin cancer
- Fungal infection
- Chronic ingrown nail
- Other health problems
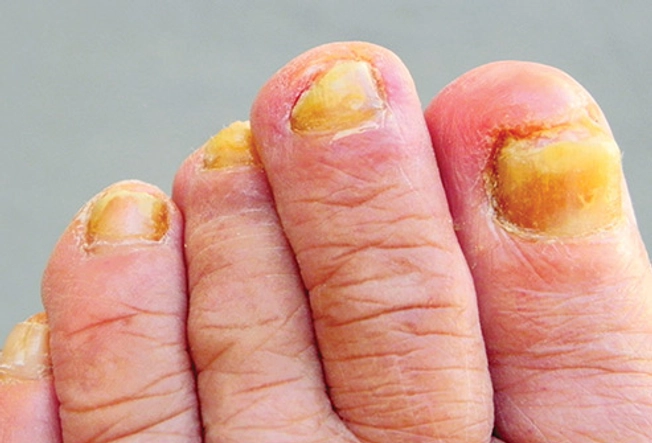
All-yellow Toenails
4/11
When toenails turn yellow, a fungus is usually to blame. This type of fungal infection is so common that you might not even need to see a doctor for treatment. Try an over-the-counter antifungal cream. If your nail is yellow and thick, gently file down the surface so that the drug can reach deeper layers. If at-home treatment doesn’t work, a doctor visit is in order.
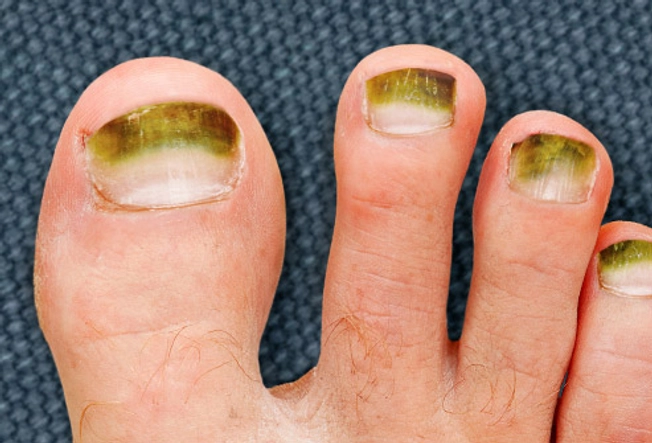
Got Green?
5/11
Unless you’re wearing green nail polish, this is a color you don’t want to see on your toenails. It could be green-nail syndrome (chloronychia), which is caused by an infection. The culprit is usually bacteria that thrive in damp or wet conditions. Think hot tubs, sponges, even tight-fitting shoes that you’ve worn for a long time. The color is underneath the nail, so don’t try to scrub it off. Visit your doctor instead.

Shades of Blue
6/11
If you stub your toe and it turns blue, you might not think twice about the color. But if you get a blue spot or a blue toenail for no clear reason, play it safe and see a doctor. You may have a blue mole beneath the nail. It’s probably harmless. But in very rare cases, a type of blue mole called a cellular blue nevus can become cancer.
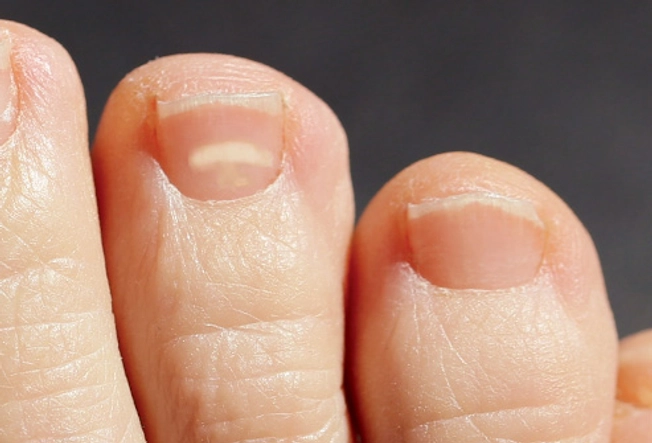
White Spots and Streaks
7/11
Stubbing your toe doesn’t always lead to a bruise. That’s because the blood vessels under the nail might not break and leak blood. Instead, you might get a white spot on your toenail. It won’t don’t disappear like a bruise, but it will grow out in time. Toe trauma can also cause a white streak — though you might not know you hurt yourself. For example, it can happen when sneakers are too small and your toe hits the front of the shoe.

White All Over
8/11
Do you have a toenail that’s turned white, or has large powder-like patches? You could have a fungal infection, most likely one called white superficial onychomycosis. If possible, see a doctor as soon as you notice it. This infection spreads across the toenail. White superficial onychomycosis can cause the entire nail to become rough and crumbly.
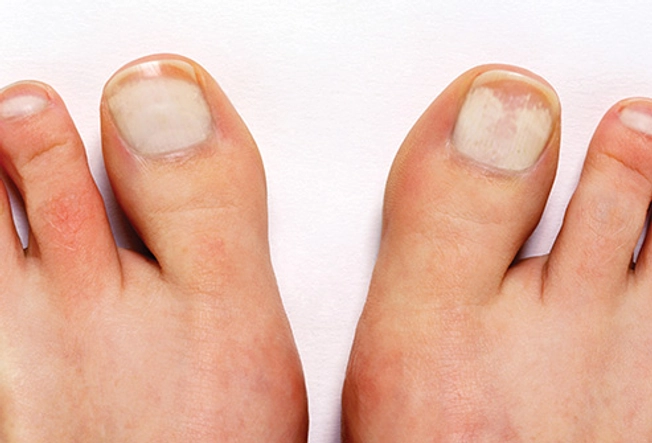
Whitish or Yellowish Patch
9/11
Another type of fungal infection is called proximal subungual onychomycosis. It looks like a whitish or yellowish patch that starts at the base of the toenail, near the cuticle. The infection is rare in healthy people. More often, it happens in people with weakened immune systems. It can also be a sign of HIV.

Candy Cane Stripes
10/11
When toenails have red and white stripes, there are usually problems elsewhere on your body. These lines and V-shaped nicks are a hallmark of Darier disease. It’s an inherited disease, mostly affecting the skin and causing greasy, warty, foul-smelling blemishes.
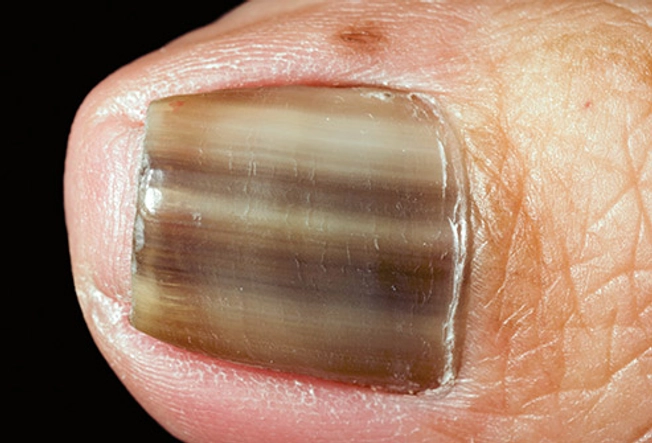
Brown Streaks
11/11
The term for brown and sometimes black color on your toenail is melanonychia. Brown usually appears as a line or streak going up and down the nail. Possible causes:
- Injury
- Melanoma
- Inflammatory conditions
- Fungal infections
- Certain medications
Because there’s a small chance your brown toenail streak could be a sign of something serious, play it safe and get checked out.
Show Sources
IMAGES PROVIDED BY:
1) Daiva Boguckiene / EyeEm / Getty Images
2) amesy / Getty Images
3) Manuel Faba Ortega / Thinkstock
4) SandroSalomon / Thinkstock
5) benstevens / Thinkstock
6) poco_bw / Thinkstock
7) RoniMeshulamAbramovitz / Thinkstock
8) ISM / Medical Images
9) Gary Ombler / Getty Images
10) Bhownit Singh / EyeEm / Getty Images
11) DR P. MARAZZI / Science Source
American Osteopathic College of Dermatology: “Green Nail Syndrome,” “Subungual Hematoma.”
The Australian Journal of Dermatology: “Subungual and periungual congenital blue naevus.”
American College of Foot and Ankle Surgeons: “White Toenails,” “Black Toenails.”
American Family Physician: “Treating Onychomycosis.”
U.S. National Library of Medicine: “Darier disease.”
Mayo Clinic: “Nail fungus.”
A Black Spot Under The Toenail: What Is It?
Under normal circumstances, our toenails are a glassy, somewhat opaque colour. The protective proteins of our toenails, called alpha-keratin, create this consistency. Together with the skin below it, healthy toenails should be pink. Sometimes, however, our toenails change colour. But why? You may experience toenail discolouration from damage to the toenail itself or from damage to the skin below the nail bed. In both instances, a black spot may appear. It can be a black spot below the toenail, or your toenail itself may change colour. This article teaches more about black spots under toenails, different kinds of toenail discolouration, and treatments. First, let’s explore the nail condition of a black toenail.
What’s a black toenail?
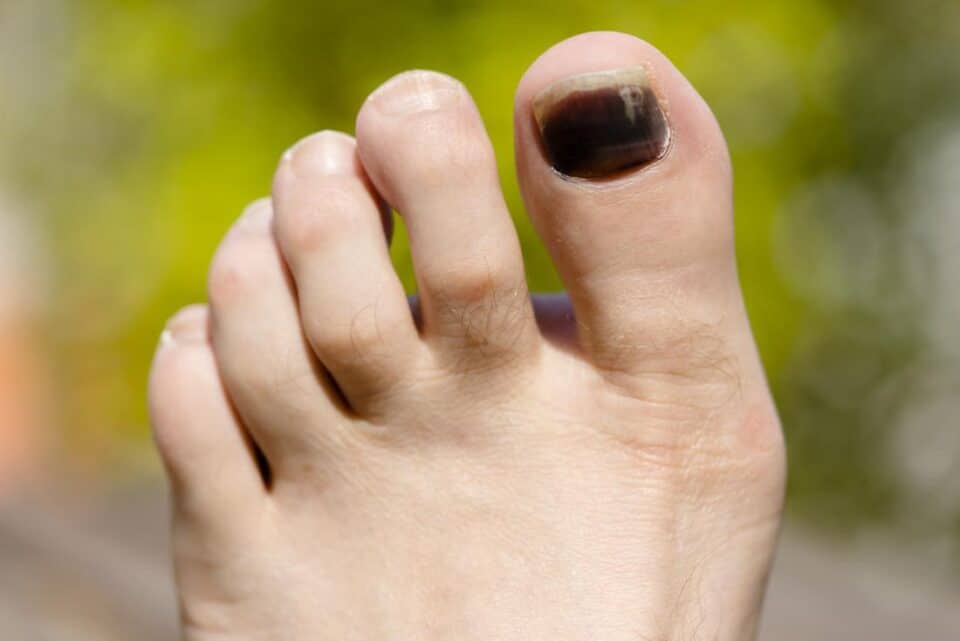
Black toenails are a type of nail condition characterized by damage to the skin below the nail. In most cases, a black toenail is a subungual hematoma, especially if you see a black spot. The black area you see is a bruise (a blood vessel breakage causing bleeding near the skin surface.) However, your toenail may turn black for other reasons. We break down the causes below.
Should I be worried about a black toenail?
Black toenails have several causes, some more common than others.
Common causes
- A subungual hematoma is the most common cause of a black spot under your toenail. Trauma, whether acute or chronic, causes a black spot under your toenail. Instances like running with ill-fitting footwear, stubbing a toe, or dropping an item on your toe are common culprits. Due to its length and weight-bearing role, your big toe is the most common toenail for a subungual hematoma. Your toenail may fall off entirely, or you may experience a small black spot. If the latter, you can trim off the black area as your nail grows out.
- You may associate a fungal infection with discolouration of the toenail. Although usually a yellow-green, your toenail may also turn black.
- In rare cases, ingrown toenailscan be the culprit for a black toenail. An ingrown toenail causing a black toenail is usually related to a complication of a previous toenail treatment.

Rare and more severe causes
- Malignant melanoma can cause a black toenail: Cancer forms in the cells of our skin that give our skin colour, which causes a black spot.
- A B12 deficiency : B12 keeps your nails strong and healthy. A lack of B12 may result in a blackish tint.
- Kidney problems
- Liver disease
- Linear melanonychia can cause black and brown lines that run either with your toenail or horizontally across your toenail.
If you have doubts about the black spot under your toenail, book an appointment with a chiropodist for the next steps and a diagnosis.
What kind of discolourations of a toenail are there?
In addition to black toenails, you may experience other discolouration. Click here to learn about the various shades and causes of discoloured toenails.
How can I treat a discoloured (including a black) toenail?
If you can connect the cause of a black toenail to a common cause—for instance, a stubbed toe—then at-home treatments are sufficient. However, if you haven’t had any trauma or damage to your nail, consult a medical professional for treatment options. Here are some ways you can treat a discoloured toenail:
Let it grow out
If your toenail isn’t damaged or at risk of falling off, the most effective action is to let the toenail grow out. Expect to wait between 6-9 months to allow your toenail to grow out thoroughly and to be able to trim the black area away.
Cover the toenail
If your toenail dies and falls off, you should cover any exposed parts of the nail bed for 7-10 days. Coat the area with a non-stick bandage and wait for the skin underneath to harden. Once the skin hardens, you can leave the nail and allow it to grow back or use an artificial nail to improve aesthetics.
Visit a chiropodist or foot doctor
If you have damage to your toenail from trauma and need guidance and treatment, visit a chiropodist. Our team of dedicated licensed chiropodists is committed to providing quality care and services for all your foot and ankle needs. They can diagnose, treat and help manage various foot conditions, from callus removal to ingrown toenails to bunions.
Over-the-counter creams and ointments
Ointments and creams are usually effective and can help treat fungal infections. You can also use a prescription antifungal treatment for severe cases of toenail infections.
Buy a new pair of shoes
If you have poorly-fitting shoes causing stress to your toenail, invest in proper footwear for your feet.

Your toenail solutions live here
All under one roof. Our team is trained to handle any and all your foot health concerns. Call us at 416-769-3338 or Book Your Assessment Today!
Related Services & Conditions
Discoloured Toenail
Ingrown Toenail
Fungal Toenail
Nail Care & Treatment
Newsletter Signup
Get biweekly health information and advice from our experts.
Related Posts

February 6, 2023
Common Foot Conditions in the Elderly and How to Treat Them
Age is just a number, but age starts to catch up with us at a certain point. As much as we want aging to slow, getting older comes with its fair share of aches and pains. Few people age the same; it is a complex process. Environment, genetics, exercise, and many other factors mould who we become as we enter our elderly years. This also applies our feet. As we age, our feet become more susceptible to various conditions such as arthritis, plantar fasciitis, bunions, foot injuries and chronic pain. Our latest blog is all about common foot conditions in the elderly and how to treat them. What happens to our feet as we age? Did you know that when you turn 70, you’ll be 25,550 days old? That helps put the body’s remarkable ability to withstand constant wear and tear into perspective. Beyond just a number, there are also physiological changes that occur as we age. Your feet may get bigger. Your feet may widen. Muscles, tendons, and ligaments also wear down, putting you at greater risk of certain foot conditions. You may notice you experience foot pain and other problems more often. Any number of the following may happen: Weakness Frailty Exhaustion Gait alteration Balance difficulties Increased swaying while walking Decreased walking Walking speed As we age, it’s essential to check how you feel regularly. A bonus would be to have your feet checked regularly. Our team of expert foot specialists can help you manage acute and chronic conditions that affect the toes, feet, and ankles. Most common foot conditions in the elderly Foot conditions amongst the elderly may include bone injuries, toenail damage, foot deformities, and muscle and tendon damage. It’s important to note that most of these conditions are not specific to the elderly, but age contributes to increased risk. Below we break down the following common foot conditions in the elderly and how to treat them: Bunions Osteoarthritis Fat Pad Atrophy Thickened or Discoloured Toenails Gout Plantar Fasciitis Stress Fractures 1. Bunions What are bunions? A bunion is a deformity of the first metatarsophalangeal joint (“MTP” joint for short). The first MTP is the joint of the big toe. (Essentially, the big toe’s “knuckle.) Damage to this joint can cause bone misalignment over time. Eventually, the bone shifts and protrudes at the base of the big toe. Bunions affect approximately one quarter to one third of adults, and women experience the foot condition more often than men. As we age, bunions worsen. Although there is no “cure” for a progressive foot deformity, you can lessen the effects and pain associated with bunions through several habitual changes. How can I treat bunions? You can choose either invasive treatment or non-invasive bunion treatment. In most cases, you can manage bunions with non-invasive treatments, though surgery is the only way to remove the bump altogether. Footwear modification: Avoid tight shoes that squeeze the toes and ditch your high heels. You may also find that orthopedic shoes that stretch or come in wide widths effectively accommodate your bunion in your footwear. Shoe stretching is also an effective method for changing the structure of your current footwear. Anti-inflammatories: Specific medication like NSAIDs or ibuprofen reduces joint inflammation and relieves pain. Splints/aligners: Medical-grade bunion splints and bunion aligners help stabilize the joint. You can choose from medical-grade plastics or a toe sleeve based on your preferred rigidity. Taping: A specialist tapes the joint to keep the big toe in place, prevent further misalignment, and manage pain and inflammation. Supportive insoles or custom orthotics: Supporting your arches and correcting poor biomechanics can reduce pressure and strain on the first MTP joint. Bunion exercises: Basic exercises to strengthen foot muscles can better support and stabilize the joint, thus decreasing pain over time. The treatments you see above are all available at Feet First Clinic. 2. Osteoarthritis What is osteoarthritis? Osteoarthritis is not only the most common variant of arthritis; it is also one of the most common foot conditions in the elderly. Osteoarthritis is the “wear-and-tear” arthritis that causes degeneration of the cartilage in our joints. Reduced cartilage in our joints causes pain and can lead to other foot conditions like bone spurs. Your toes are most susceptible to osteoarthritis. Age plays a significant role in developing osteoarthritis. Wear and tear of our joints accumulate over time. Also, post-menopausal women risk developing osteoarthritis through osteoporosis (low bone density). How can I treat osteoarthritis? Osteoarthritis is a degenerative condition, meaning what’s done cannot reverse. The cartilage in your joints doesn’t re-grow, so treatment aims to slow the effects of osteoarthritis and reduce pain. Effective treatment includes a combination of the following: Active rehabilitation: Physiotherapy, massage, and exercise all help reduce the effects of osteoarthritis by promoting solid muscles. Stronger and more balanced muscles and feet reduce the strain on affected areas where you may have osteoarthritis. Medication: Anti-inflammatories can help control inflammation. Proper footwear: Specialized shoes can accommodate deformities of osteoarthritis (like bunions or hallux rigidus). The right shoes or boots can support your feet, provide balance, and offer cushion. Custom orthotics: Orthotics can be customized to add or reduce your reliance on certain parts of your feet. Controlling the impact on affected joints can help prevent further joint damage by distributing the impact and weight elsewhere. Limit awkward movements: If you find your joints are sore after a particular activity, consider reducing, modifying, or stopping the activity. For instance, if lunges hurt your foot, consider finding a replacement exercise. Surgery: If the joint is damaged extensively, a doctor may recommend surgery. Surgery and removing part of a bony outgrowth can be effective if the sheer volume of bone buildup is the culprit. If you experience osteoarthritis and are looking for orthotics, a gait analysis, or proper footwear, visit Feet First Clinic for solutions. 3. Fat pad atrophy What is fat pad atrophy? The heel fat pad is a cushion to absorb shock and distribute plantar force on impact. As we age, the heel fat pad gets atrophies and gets thinner. This can put you at a greater risk of heel injuries and other foot conditions. The increased pressure on the heel can cause you to overcompensate with other parts of your body, and weight distribution becomes unevenly distributed. How can I treat fat pad atrophy? You should reduce the pressure on your heel if you suffer from fat pad atrophy. Custom orthotics are effective as the personalized insoles provide padding and support and help distribute weight across the complex network of foot muscles. Be sure to also wear shoes with lots of padding and cushioning, like the ASICS Gel-Nimbus. 4. Thickened or Discoloured Toenails What are thick or discoloured toenails? Thick toenails and discoloured toenails are a byproduct of aging and are one of the most common foot conditions in the elderly. As we get older, toenail growth declines. As such, nail cells begin to accumulate at a faster rate than nail growth. The accumulation of onychocytes (nail cells) causes thickened toenails. Alternatively, reduced circulation or acute trauma can cause thickened toenails. Discoloured toenails, on the other hand, indicate damage to the nail or nail bed. Acute trauma to the nail causes discolouration, but so does reduced circulation. At an older age, we’re at a greater risk of diabetes and peripheral vascular disease. Both diabetes and peripheral vascular disease cause reduced circulation in our feet and discoloured toenails. How can I treat thick or discoloured toenails? Toenail treatment for thickening and discolouration varies. To properly diagnose your feet and nails, book an appointment with a specialist at Feet First Clinic. Our nail care services involve proper trimming and filing of the toenails, addressing any pain or discomfort, and educating patients on proper hygiene and
care. For more information, visit our nail care and treatment page. 5. Gout What is gout? Gout is a form of inflammatory arthritis targeting the foot’s joints. You may experience intermittent bouts of severe pain, including inflammation and hypersensitivity. During these episodes, any kind of activity becomes challenging, leaving you less mobile. The prevalence of gout increases in older people. Elderly people are susceptible to gout for a few reasons: Renal function declines with age, there can be dietary changes, you may experience sudden weight gain, and certain medications for age-related conditions have indirect side effects that may lead to gout (i.e.: water pills, blood pressure medication). How can I treat gout? Before any treatment, the first step is to see a family doctor and a rheumatologist. Once diagnosed, you may be prescribed the following treatments, all of which aim to prevent future attacks, reduce pain, and improve quality of life: Change your diet: Ditch food containing excessive purines. Avoid foods like red meat, certain types of seafood like sardines and mussels, alcohol, high fructose beverages, and yeast. Diet also impacts your weight. Maintaining a healthy and consistent diet can help reduce sudden weight gain and keep inflammation at bay. NSAIDs: Non-steroidal anti-inflammatory drugs reduce joint inflammation. Alternatively, corticosteroids are an option if one doesn’t react to NSAIDs. Stay or become active: Light-strengthening exercises, relaxing physical activity, and physiotherapy can improve quality of life and mobility in people with gout. Keeping your muscles strong also makes them less susceptible to inflammation build-up, which can trigger gout attacks. Supportive footwear: Proper footwear can help you deal with any pain associated with gout as it reduces the impact on the joints. 6. Plantar fasciitis What is plantar fasciitis? Plantar fasciitis is a condition of the heel. The band of tissue on the underside of the foot gets inflamed and causes pain. Often, plantar fasciitis develops gradually over time. Changes in our body as we age can make this condition more common in the elderly. How can I treat plantar fasciitis? With proper care and treatment, most cases of plantar fasciitis heal with time. A foot specialist can guide you through the healing process and provide options for preventing it from recurring in the future. There are several treatment methods available for plantar fasciitis. Rest: Take a break, and let your heel recover by staying off your feet. Supportive footwear: Wearing supportive footwear with strong arch support and a good heel counter is essential for managing and even preventing plantar fasciitis. Stability shoes are particularly helpful. Check out this article for our top recommended shoes for plantar fasciitis. Rolling: Gently massage your heel using a tennis ball or frozen water bottle under the foot. Rolling helps massage and relieve the plantar fascia and encourages faster recovery. Add stretching and strengthening exercises to your routine. Shockwave therapy: Shockwave therapy delivers sound wave pulses to the injured fascia. This triggers your body’s the healing process, making for a natural recovery. Shockwave therapy is extremely effective for cases of plantar fasciitis persisting more than 6 months. Taping: Taping the heel engages other muscles and tendons of the foot, reducing the load on the plantar fascia. Wear a splint: A splint helps keep your foot stable while you sleep. Supportive Insoles or Custom Orthotics: A good supportive insole, like Superfeet Green, is tried, tested and true for helping with plantar fasciitis. If that doesn’t work, or if there are biomechanical factors contributing to your plantar fasciitis, you can look into custom orthotics. 7. Stress fractures What are stress fractures? Stress fractures are micro-breaks of bones are another common foot condition in the elderly. When we age, bone growth slows, losing more bone than we generate. Our bone density also reduces. If your bone density drops too much, you develop osteoporosis. Weaker bones put the elderly at greater risk of stress fractures, whether acute, like when you fall or by too much repetition, like walking. How can I treat a stress fracture? The RICE method is critical to treating a stress fracture. Rest, ice, compression, and elevation. Untreated stress fractures can lead to bone shift, permanently altering the foot’s biomechanics.
January 23, 2023
Beau’s Lines on Nails: Causes, Symptoms, Treatment
Have you ever noticed horizontal lines or grooves lengthwise across your nails? The nail abnormality is called Beau’s lines. You may develop Beau’s lines after trauma to the nail, or it may be a sign of an underlying medical condition. Today’s blog article explores Beau’s lines, potential causes, and treatment methods. Keep read to learn more about Beau’s lines and how to keep your nails healthy and strong. What are Beau’s lines? Beau’s lines are a type of nail abnormality. They are indentations, grooves, or lines that run horizontally across the nails. The condition can affect any number of fingernails or toenails. Amongst your toenails, the big toe is the most common culprit. Curious as to why they’re referred to as Beau’s lines? French physician Joseph Honoré Simon Beau first discovered the condition, hence the name. What causes Beau’s lines on nails? A temporary disruption in the growth of the nail matrix causes Beau’s lines. They are symptoms of an underlying illness, medical, or skin condition. They appear when average nail growth is interrupted, and the blemishes appear due to irregular keratin (skin cells) development. Once you can identify and treat the underlying cause, normal nail growth may resume. Identifying Beau’s lines can be delayed because of the nail growth rate. Toenails grow at ~1.60 mm per month, so nail growth delays Beau’s lines’ arrival. The lines appear roughly 2-3 weeks after damage or cause sets in. The number and distinctiveness of Beau’s lines can provide insights and clues into possible causes. For instance: One Beau’s line on a single toenail may indicate a less severe injury. Beau’s lines on multiple nails may indicate higher stress levels or a more severe injury/illness. Several rows of Beau’s lines on each toenail with a gap in between may indicate multiple traumas over time, but not at once. Fewer but thicker Beau’s lines may signify a chronic injury or illness. Beau’s lines may occur for several reasons. Possible causes include: Illness or severe stress. Being ill or stressed can divert your body’s resources and nutrients away from nail growth. Blood flow interference due to an illness or infection is the culprit. Certain illnesses or infections can cause Beau’s lines, including: Viral infections Heart attack High fever Measles Mumps Pneumonia Strep infections Raynaud’s disease COVID-19. A study published in the National Library of Medicine noted that COVID-19 might cause Beau’s lines. The coronavirus is by no means the sole cause of Beau’s lines but can be a trigger. As such, Beau’s lines are sometimes known as “COVID nails.” Nail trauma. Acute or chronic trauma to your toenails can interrupt nail growth and cause Beau’s lines. For example, you may stub your toe, drop an item on your foot, or wear ill-fitting shoes that add undue pressure to your toes and toenails. Damage to the nail matrix—the part of the nail where growth starts—is notably correlated with Beau’s lines as growth is interrupted at the root. Skin conditions. Skin conditions, including eczema and psoriasis, can damage your nail matrix. Vitamin or nutrient deficiencies. Particular vitamin and nutrient deficiencies can interrupt nail growth. For instance, biotin deficiency is known to cause brittle nails and affect nail growth. Zinc deficiency is also linked to the nail condition. Chemotherapy side effects. Approximately 23% of anti-cancer therapy patients report nail changes. Changes to the nail may include Beau’s lines. Paronychia. Inflammation of the skin around the nails (known as paronychia) can cause Beau’s lines. How do I treat Beau’s lines? Moisturizing dry, itchy skin, both the byproducts of skin conditions, can help reduce the damage to the nail fold. There is no one-size-fits-all treatment for Beau’s lines, nor is there a specific treatment for the condition per se. The key is to address the underlying cause – whether it be a medical condition or acute trauma – rather than the symptom (i.e.: what you see on your nails). Below are several possible treatment methods you can try, depending on the underlying condition: Allow the nail to grow out. Nail growth is approximately 1 mm every 6-10 days. Letting the nail grow and slowly trimming the tips reduce the appearance of lines on the toenail. The entire toenail should grow out within 6-8 months. Apply creams or moisturizers for eczema or psoriasis. Moisturizing dry, itchy skin, both the byproducts of skin conditions, can help reduce the damage to the nail fold. Avoid salon manicures, artificial nails or harsh nail products. Avoiding harsh chemicals and products can help reduce the trauma of the nail matrix. Mask the ridges with nail polish. Nail polish is a cosmetic treatment to hide the grooves from Beau’s lines. However, some nail polishes can weaken the nail, so be cautious about your product. Get a medical pedicure from a licensed chiropodist to encourage proper nail growth, perform a thorough examination, and eliminate onychophosis (the buildup of skin cells in the nail folds, nail plate and cuticles). Take biotin supplements. Some studies suggest that taking biotin can increase nail plate thickness by 25%. Generally, adults 19+ should be consuming 30-35 mg of biotin per day. Biotin and Zinc supplements are believed to help nail growth. If you find Beau’s lines persisting, or worsening, it’s recommended to contact a healthcare professional for a proper diagnosis and treatment plan.
January 16, 2023
Toenail Pitting: What is it?
Fact: Your toenails can give you clues about your overall health. That’s right, the state of your nails, including toenails, can indicate an underlying health condition. Conversely, healthy nails can be a sign of a healthy lifestyle. The state of our toenails can differ in a lot of ways. Toenails can splinter, thicken, thin, peel, dry out, break, and pit. Toenail pitting is the focus of this article. Below, you’ll learn about toenail anatomy, the basics of pitting, signs, treatment methods, and preventative measures to keep your nails in good shape. Toenail anatomy Before we delve into the details of toenails and pitting, we must understand their anatomy and the part it plays for our feet. Toenails are the plate-like covers on our toes. Alpha-keratin, a type of protein, comprises toenails. Alpha-keratin is the same protein building block for hair and the outermost layer of our skin (the epidermis). Generally, the toenail is about 0.5 mm thick and slightly curved. The toenail consists of several distinct components. The toenail includes the nail plate, the cuticle, and the nail folds surrounding the nail’s perimeter. The part referred to as the toenail colloquially is the “nail plate.” What’s toenail pitting? Pitting, by definition, is an indentation. Toenail pitting follows the same logic. Pitting of the nail occurs when tiny dents or “pits” form in the nail plate. Toenail pitting is a type of nail abnormality. Toenail indents can be shallow and only recognizable by touch. Deep toenail pits may be visible due to their concave nature. Within the grooves, some parts of the pitting may be deeper than others, just as there are deeper and shallow parts of a pit. Nail pitting is generally more common for fingernails, but toenails are also affected. What causes toenail pitting? There are several causes for toenail pitting. Toenail pitting reasons range from external trauma to an underlying medical condition. Learn about the various causes of toenail pitting below. Nail psoriasis Psoriasis is a chronic inflammatory disease that can cause toenail pitting. Those with nail psoriasis produce too many skin cells, causing nail irregularities. According to Healthline.com, approximately 80% of those with psoriatic arthritis experience nail irregularities or changes. You may be able to recognize nail psoriasis because of two related symptoms: discolouration and nail bed separation. There are a few groups more likely to develop nail psoriasis. At-risk factors include: People who are over 40 (though psoriasis may occur at any age) Males Genetics Psoriatic arthritis According to a study published in the National Library of Medicine, psoriasis can cause toenail pits “remarkably even in size and depth. Their distribution may be haphazard or sometimes arranged in parallel transverse or short longitudinal lines.” Though psoriasis is not curable, you can mask the effects of toenail pitting. You can buff or apply nail polish to hide the indents and improve the aesthetic. Nail eczema Eczema is a condition that causes itchy and red skin. The disease can cause nail thickening or pitting when eczema targets the feet. Habit-tic deformity Habit-tic deformity on the fingernail. The habit-tic deformity is a nail condition similar to toenail pitting with several differences. When you constantly pick at your nails, external trauma can create pits in your nail. The habit-tic deformity is most common on the fingernails, specifically the thumbs, but it can also happen on your toenails. For instance, if you sit cross-legged or have your feet at arm’s reach, you may develop a habit of picking at your toenails. The defining features of habit-tic deformity are horizontal ridges across the nail and a slight depression in the middle of the nail plate. The habit-tic deformity is not severe and typically heals if left alone. The condition is known as “washboard nails” because of the horizontal nail ridges. Reiter’s syndrome/reactive arthritis Those with reactive arthritis may experience toenail pitting. An infection or bacterial infection elsewhere in the body can cause reactive arthritis, also known as Reiter’s syndrome. People with a specific type of gene are more likely to develop the condition, as it’s believed to be genetic. How do you fix nail pitting? Toenail pitting fixes vary. In some cases, like psoriasis, there is no cure. Cosmetic procedures are an option to mask the effects. Removing external trauma can help reverse toenail pitting in cases like a habit-tic deformity. Additional treatment options include medication applied to the nail itself. Options include steroids, salicylic acid, calcipotriol, cyanoacrylate adhesive (for the habit-tic deformity) and tazarotene. Is nail pitting serious? In most cases, nail pitting as a symptom isn’t severe. Nail pitting is more often a cosmetic issue than a medical issue. However, the underlying conditions that cause toenail pitting can vary in severity.

January 9, 2023
Red Toes: Should You Worry?
There can be a range of discolouration in your toes. The most common is a pinkish/red hue – a sign of red toes. Red toes may result from cold temperatures, toe injury, infection, or potential medical conditions. Red toe onset may be immediate, or red toe onset may be progressive. The redness often resolves itself, but it may sometimes present symptoms of underlying medical conditions. Learn more about red toes and potential risks in our article below! Why are my toes red and itchy? Several causes result in redness in your toes. Red toes result from inflammation, injury, temperature, skin irritation, and infection. Varying degrees of redness may indicate the severity of damage to the toes. In some cases, redness may subside independently, while others may require medical attention. What medical conditions cause red toes? There are a variety of medical conditions that induce red toes. Red toe causes range from skin conditions to musculoskeletal damage to infection. Below, we’ve categorized medical conditions that cause red toes by severity. Note that all medical conditions can have varying degrees of severity, so use this list as a reference, not a diagnosis. Lower severity Low-severity medical conditions that cause red toes are short-term causes and often subside independently. Proper attention and care are required to prevent additional damage. However, low-severity medical conditions that cause red toes are more surface-level and less cause for concern. Blisters A blister is a small fluid-filled bubble that forms just under the outer layer of the skin. The fluid (usually a serum, rarely blood) is a natural cushion to protect the tissue underneath from friction and irritation. Fortunately, blisters often heal on their own once the source of friction is eliminated. As tempting as it may be, avoid popping the blister and allow it to heal naturally. Frostnip Frostnip is a mild, non-severe cold injury to the skin and tissue. As such, frostnip doesn’t cause permanent damage. You can treat frostnip with basic first aid. Above all else, you should try to escape the cold as quickly as possible. Possible complications include infection and temporary nerve damage, which are rare if caught at the frostnip stage. Stubbed toe A stubbed toe occurs any time you jam your toe against another object. A stubbed toe is a trauma injury. The injury results from a one-time accident. Depending on the severity, damage to the toe may cause swelling and inflammation, muscle injury, and even bone fractures. Contact dermatitis Contact dermatitis is a red, itchy rash triggered by an allergic reaction. The skin’s response to an irritant causes inflammation, followed by a rash. Contact dermatitis isn’t contagious nor life-threatening, but it can be very uncomfortable. Soaps, plants, detergents, or jewelry have the potential to cause an allergic reaction. One can treat and prevent contact dermatitis by identifying and removing environmental allergens. A doctor can also prescribe topical medications to help treat flare-ups. Athlete’s foot Fungal skin infections are a common culprit of red toes. Athlete’s foot is one such common fungal skin. Athlete’s foot is a prevalent cause of the redness. The toe fungus is not life-threatening, but it is contagious and may spread elsewhere on your body or even to other people. It can also cause foot pain and difficulty walking if left untreated. Nail infection Paronychia is an infection of your nail folds typically caused by bacteria or a fungus and can cause toe pain and swelling, which causes redness and the appearance of red toes. Ingrown toenail An ingrown toenail is a nail condition that targets the toes, mainly the big toe. As the name applies, it occurs when the sides or edges of the toenail grow into the skin. As the nail pierces the skin, it can cause bleeding, redness and pain. If left untreated, the ingrown toenail can get infected. Moderate severity Moderate-severity causes of red toes are more severe and may be longer-lasting. Symptoms and recovery time may vary, and pain and discomfort may be more intense and significant. You may require medical assistance to determine the diagnosis and treatment method(s). Gout Gout is a form of inflammatory arthritis caused by heightened uric acid in the blood. Elevated uric acid levels lead to the formation of crystal deposits in the joint. The joint then becomes red, hot, swollen, and painful. The initial attack of this condition is usually sudden, with symptoms lasting for about a week. The most common joint it affects is the joint that connects your big toe to the rest of the foot. If left untreated, gout attacks may reoccur, increase in severity and lead to enduring joint damage. Frostbite (superficial) Superficial frostbite is a stage more severe than frostnip. Cold temperatures damage the skin and the underlying tissues in your toes. Blisters form 24-36 hours after rewarming, and you may experience pain and discomfort for several days. Higher severity More serious medical conditions that cause red toes may be chronic or permanent. These conditions can be irreversible and limit the motor function of your toes. Surgery may be a last-resort treatment option in severe cases. Rheumatoid Arthritis Rheumatoid arthritis (“RA”) is an auto-immune disease that causes chronic joint inflammation. RA causes periodic flare-ups of joint pain, stiffness and swelling, eventually making movement difficult. Although there is no cure, you can manage the condition with proactive and diligent treatment focusing on your overall health and well-being. Diabetes Diabetes can cause a chain reaction in your body that hinders circulation to the feet and toes. People with diabetes may experience two conditions that cause red toes: peripheral vascular disease and nerve damage (diabetic neuropathy). Nerve damage and reduced circulation can cause an itchy or numbing pain in the toes. Diabetes can also hinder the body’s ability to fight less severe conditions due to reduced immune response and blood circulation. Frostbite (deep) Deep frostbite is the most severe form of cold damage to the skin. Your skin or tissue may turn red and black and die altogether. You may sometimes lose muscle function and require surgery to remove part of the toe. Bunions A bunion is a foot condition of the first metatarsophalangeal joint. Bunions occur when the big toe misaligns. The shift in bone structure causes what appears to be a bony outgrowth. The outgrowth is simply the angling of your toes. The damage to the joint causes pain and redness, and the increased volume of your toes can make wearing shoes uncomfortable. Without proper footwear or orthotics, you can further aggravate your bunions. Bunions are irreversible and have no “cure” other than surgery. However, physical therapy and accommodations, like orthotics and proper footwear, improve quality of life. How can I prevent my toes from turning red? Treatment and prevention for red toes depend on the severity of the underlying medical condition. Generally, low-severity medical or skin conditions are treated simply through rest and recovery. For low-severity conditions, the goal should be to focus on “How do I prevent this from getting worse?”; whereas for high-severity needs, much of the damage has been done and is irreversible. For more severe red toe conditions, the focus is more geared towards improving quality of life and implementing tools to improve mobility, like custom foot orthotics or orthopedic footwear. We’ve created a treatment guideline below: Low severity. Low-grade medical or skin red toe conditions are treatable, often at home. Treatment methods include topical creams or prescription medication, rest, recovery, taping, or changing footwear. Further prevention should focus on recognizing signs and symptoms of red toes early and following proper foot hygiene. Moderate severity. Moderate severity medical or skin red toe conditions are a mix of prevention and treatment. A proper diagnosis is often required, followed by a treatment plan. Rest and recovery may be part of the treatment plan, but the recovery may be longer (weeks, not days). Like low-severity ca
uses, prevention should focus on recognizing signs and symptoms of red toes early and following proper foot hygiene. Higher severity. Severe medical or skin red toe conditions are often irreversible and have no cure. Treatment methods focus on improving motor function, mobility, and well-being through orthopedic tools and physical therapy.

November 17, 2022
Learn How a Foot Specialist Cuts Toenails
A self-performed nail trim may seem like a simple task. However, many people make plenty of mistakes when trimming their nails. Failing to follow the correct technique can lead to a wide array of painful toenail problems, like ingrown toenails (P.S. you should never try to cut your own ingrown toenails), cracked toenails, and even infections like toenail fungus. In the world of podiatry and chiropody, a trim nail is serious business. There are guidelines to follow to protect your toenail health, and foot specialists also recommend specific tools of the trade. The good news is you can learn to trim your toenails properly from home. Let’s look at common toenail trimming errors (and useful tips) and then learn how to cut your toenails like a pro! Toenail Trimming: Common Errors and Helpful Tips Don’t trim your toenails when they are wet. Everyday Health notes you should trim them while dry for a smoother cut. Don’t clip your toenails too short. This almost guarantees ingrown toenails, as the skin can overlap the toenail. Use the right toenail clippers and avoid using unusual objects for toenail trimming, like standard scissors. Curving the edges of your toenails may look aesthetically pleasing, but experts suggest not doing this. It will put you at risk of ingrown toenails, so trim your toenails straight across instead. Clip your toenails every six to eight weeks. Don’t wait longer, or it will be more difficult. Athletes may want to clip more frequently. Maintain a toenail length of 1 to 2 mm, no shorter. Toenail growth can be quite slow sometimes. If you don’t have the right tools, enough time, or simply the confidence to focus on a nail trim, try a medical pedicure instead. It includes the right nail trimming procedure and concludes with a relaxing (and beneficial) moisturizing session, thorough cleaning, and more. Before the nail trim, a chiropodist also examines your feet for other foot conditions. Try OnyFix if you’re already burdened with ingrown toenails. This non-invasive, pain-free procedure ensures your toenails grow in the right direction. How a Foot Specialist Cuts Toenails Start with a clean, dry base. A clean base keeps your tools from slipping and eliminates debris so you can see the toenails clearly. Cut your toenails after a shower or bath and ensure they’re dry, using a towel to soak up any excess water. Use sharp nail clippers or nickel-plated pedicure scissors. Remember, toenails are thick, so flimsy tools will just cause mistakes. Clip nails straight across. There should be no curving of the edges or cutting the nails down too far. A straight cut keeps the nail growing in the right direction. Trim once more if needed. If the first trim doesn’t look quite right, trim straight across one more time. Cut along the straight line of the initial cut to clean up the edges. Use a nail file. This tool is necessary for properly smoothing the edges of the nails. After the trimming, there will likely be some jagged edges, sharp corners, and “spikes.”

November 3, 2022
Top 5 Benefits of Medical Pedicures
Medical pedicures are no ordinary cosmetic pedicure. And while the procedure skips the pretty toenail polish, they offer numerous foot health benefits that you won’t get from your favourite nail salon and spa. Regular medical pedicures work wonders for nail health and keep your skin in good condition. What’s more, chiropodists know the warning signs of foot conditions, so they can keep their eyes peeled for potential problems while performing your pedicure. Let’s take a look at the top 5 benefits of medical pedicures! Medical pedicures prevent ingrown toenails Your chiropodist can detect foot abnormalities and conditions Say goodbye to foot odour Enjoy a thorough moisturizing session Safe and sterile environment Medical Pedicures Prevent Ingrown Toenails Ingrown toenails are something to avoid at all costs. Ingrown toenails grow into and pierce the skin, so while they may start out as a tiny problem, the pain can be immense if the ingrown toenail isn’t properly dealt with. Not knowing how to cut your toenails properly can trigger ingrown toenail growth, so you should opt for a professional trim if you don’t know what you’re doing. Of course, medical pedicures include thorough nail trimming and filing. Cutting and filing straight across ensures smooth edges and lets the nail re-grow in the right direction. This can prevent ingrown toenails but also serves as a treatment for any pre-existing ones. Bonus tip: Try researching the best toenail clippers for added protection against ingrown toenails. Your Chiropodist Can Detect Foot Abnormalities and Conditions When you get a medical pedicure, a trained professional examines every inch of your foot. This is one of the most beneficial aspects of getting a pedicure at a foot clinic vs. a nail salon. If you have diabetes, getting a foot examination is even more crucial. Due to diabetic neuropathy, irregular glucose levels, and peripheral vascular disease, undetected foot abnormalities can make way for severe complications. These may include skin and bone infections, gangrene, abscesses, and even amputations. Here are some examples of what a chiropodist can look for during a medical pedicure: Warts Corns and calluses Signs of proper blood circulation Fungal infections Nerve function Signs of additional infection Say Goodbye to Foot Odour A medical pedicure includes sanitizing and thoroughly cleaning your feet. The process starts with cleaning the feet with alcohol, so the chiropodist has a clean base. This eliminates dead skin and bacteria on the bottom of the feet, eliminating unpleasant foot odour. To ensure foot odour doesn’t come back, wash your feet regularly, wear socks with sneakers and use high-quality foot deodorants. Safe and Sterile Environment Everyone likes to feel pampered sometimes. But while salon pedicures are fun and relaxing, there can be a lack of cleanliness in some establishments. Manicure and pedicure salons can be breeding grounds for foot fungus and other concerning threats. When you go to a foot clinic, all eyes are on you. You have a space dedicated to your treatment, and your chiropodist only pays attention to your medical pedicure. Your foot specialist also uses only steam sterilized equipment that is sterilized after each use, and has plenty of time to ensure all medical practice standards are followed. But a salon may be jam-packed full of customers, and employees can easily forget to thoroughly clean tools when they’re too busy. This is when viruses, fungus and bacteria come into the picture. Enjoy a Thorough Moisturizing Session If you think moisturizing only happens at a nail salon, think again. A chiropodist will use medical-strength moisturizing creams at the end of the medical pedicure. This intense treatment works to keep skin feeling soft and clean, restore natural elasticity, and fight common nuisances like dry, itchy skin.






